TRENDS & FUTURE DIRECTION IN HEALTHCARE SERVICES
- Mona Hyder
- Dec 6, 2020
- 6 min read
Updated: Dec 8, 2020
Figure-1
INTRODUCTION
With the turn of the century, there has been a dramatic change in technology that is evolving at an exponential rate. We are seeing a rapid, emerging trend of use of technology in every field of life, especially in healthcare. Digital health tools are creeping very swiftly in our lives. Healthcare organizations need to quickly acquire and adapt to this fast-evolving technology. Although the road towards digitalization is long and full of twists and turns on unchartered grounds, as healthcare leaders, we must start preparing in order to mitigate its impact as much as possible. COVID-19 has pushed us further in adapting to new social norms and exploring new innovative ways to provide health care services.
Some of the latest trends that I will be discussing in my blog are eHealth, telemedicine, and artificial intelligence (AI) in healthcare. I will be discussing their benefits and some challenges associated with these technologies.
eHealth
eHealth or digital health is a growing trend in the field of health sciences that is believed to have changed the future of health care. It integrates information and communication technologies (ICT) to optimize clinical and non-clinical administrative services that deliver high quality patient-centric care. eHealth has a broader scoop, it improves access to health care for patients, provides training, and raises awareness to improve health outcomes.
The world health organization (WHO) defines e-health as "the safe and cost-effective use of ICTs and their role in supporting health and related areas, including health care services, health monitoring, health literature, education, and knowledge.”
Benefits
eHealth services extend beyond geographical boundaries. Services can be delivered to people in rural and remote areas, thus saving time, money, and precious lives. This technology raises awareness as it provides patients with more information about their own health. The outreach of preventive health services and programs for the vulnerable population has unlimited benefits. eHealth data collection can inform policy makers and health service providers on how to design better programs and intervention strategies.
Barriers
1- Lack of interest and lack of resources in building the ICT infrastructure and the necessary hardware and software.
2- Absence of clear vision from the healthcare leadership.
3- Lack of experienced personals who are qualified in the field of medical information technology.
4- Inadequate laws and legislations regarding the complexities and provisions of eHealth services.
5- Lack of cooperation and coordination between different sectors of health care.
Telemedicine
Telemedicine is also referred to as “remote treatment”. It is the sole delivery of health care services to patients virtually using secure video and audio connections.
Benefits
It reduces the healthcare costs and minimizes patient no shows as they don’t have to travel long distances for their appointments. It is convenient, saves time and is flexible, patients can access care in the comfort of their own homes. Lessens the time off from work, and day care costs. The outreach of this type of healthcare service is tremendous as it increases the scope and reach of health care services to remote and the vulnerable population. People in the rural areas and the underserved areas can receive quick access to specialist care irrespective of their location. It reduces department patient volume, wait times, thus reducing exposure to infections. Telemedicine also lowers the number of readmissions, ER visits, and patient transfers, ultimately reducing the medical practice overhead to lower healthcare costs.
Challenges
1- Protecting medical data from hackers, and other criminals especially when patient data is accessed through unencrypted channels.
2- In cases of medical emergencies, the healthcare provider cannot provide life saving treatments and laboratory testing with telemedicine.
3- Finding the appropriate digital platform that works for both parties can be a challenge.
4- The inability to physically examine patients can compromise the treatment.
Artificial Intelligence (AI) in healthcare
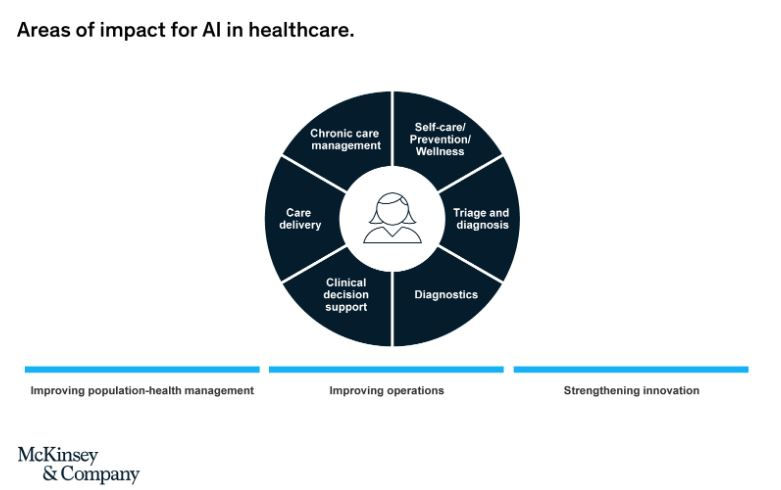
AI in healthcare is reshaping the mode of delivery of healthcare services rapidly around the world. The European Parliament in 2016 defined AI as “the capability of a computer program to perform tasks or reasoning processes that we usually associate with intelligence in a human being.” With the assistance of AI, the healthcare providers can make decisions with much more accuracy, and drastically reduce the element of human errors especially within the field of diagnosis, imaging, and developing methods for individualized medical treatment plans. AI applications based on imaging that are currently in use are in the fields of radiology, pathology, and ophthalmology.
Figure 2: An image prepared by McKinsey & Company (2020) elaborating the areas of Impact for AI in healthcare.
(Spatharou et. al., 2020)
Benefits
Automation of the most basic and repetitive administrative tasks in healthcare using AI results in quicker, better patient service, big data analysis, improve project implementation, delivery of advanced treatment, lower costs, and better medical outcomes.
Robot- assisted surgery has reduced surgery- related complications, less pain, and quicker recovery time.
Drones are being used to deliver medications, vaccines, and Automatic External Defibrillators (AED) to remote areas.
Using AI algorithms technology to pick up suspicious database activities can prevent database breaches and hacking in real time.
Video 3: This video shows the test trial using drones to deliver defibrillators to rural parts of Canada.





Comments