Multilevel Approach to Mental Illness
- Mona Hyder
- Oct 27, 2020
- 7 min read
Updated: Nov 26, 2020

INTRODUCTION
The mental health of an individual is influenced by many complex components of the world that surrounds them. Elements like socio-economic status, culture, and environmental factors can impact mental health both positively and negatively. These factors are called social determinants of health. Unequal and systematical distribution of determinants of health amongst different groups of people leads to health care inequities.
It is very important to understand the complex and multiple contextual relationships among the social determinants of health. In this blog, I will be analyzing Wider Determinants of Health Model presented by Dahlgren and Whitehead in 1991. This model identifies wider determinants and factors outside of physiology that impact health outcomes. This model is also relevant in the context of mental health.
The image below is the Wider Determinants of Health Model that examines the factors that play a role in health outcomes.
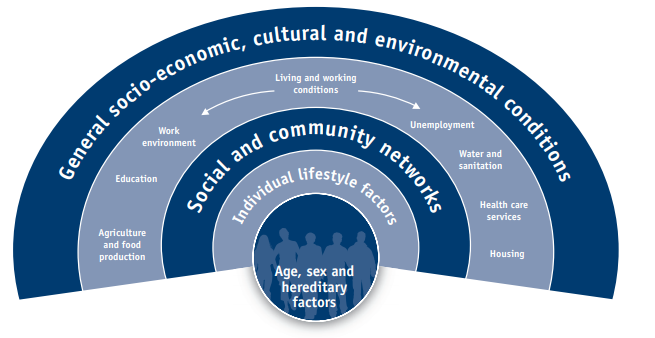
The wider determinants of health model is the most commonly used model to explain the determinants of health. It incorporates a 180 degree analysis of all the aspects of ones life. It comprises of many determinants or layers that impact health of individuals both directly and indirectly. It is composed of the following layers: constitutional, individual lifestyles, social & community networks, living & working conditions and finally the cultural and environmental conditions. This model explains the concept of health equity and its implications to develop programs and health services according to the needs of society.
CONSTITUTIONAL FACTORS
The core of this model is made up of the constitutional factors such as, age, sexual orientation, race, and ethnicity.
Age is an important factor to take into consideration in terms of identifying, diagnosing, and preparing treatment plans for individuals. There are many programs and services throughout Ontario that are directed to provide service and resources to Ontarians of different age groups.
It appears that mental illness is more prevalent in the senior population, but that is not true. There are multiple contributing factors that play a role in that age group, for example conditions like dementia, chronic illnesses, geriatric depression, dependency, and loneliness are common in the older age group. Hence the percentage of mental illnesses in older age group is higher.
On the other end of of spectrum, children that are exposed to stressful life situations, like domestic violence and abuse, belonging to the lower socio economic status, low parental education, lacking proper housing, and coming from a group that does not have access to good health care services are more prone to mental illnesses. There are multiple factors and stressors that augment each other to increase the risk developing mental illnesses.
Gender inequality has increased the rate of common mental illnesses in women. Gender is another basic contributing factor that does impact mental health in certain populations. Women are under lot of pressure due to the multiple roles they play as care takers, coupled with poverty, hunger, malnutrition, overwork, domestic violence and sexual abuse, all these factors when combined account for women's poor mental health.
The constitutional factors of this model play an important role in determining mental health of an individual. There are many other determinants or layers that also compound on this base core level. It is very necessary for the policy-makers to identify these points for interventions and service planning.
INDIVIDUAL LEFESTYLE FACTORS
The next level comprises of the individual lifestyle factors which includes personal behaviors and lifestyle choices. Examples of this are unhealthy eating habits, lack of physical exercise, inadequate sleep, addiction, and alcohol. Exposure to any kind of abuse, whether verbal, physical, sexual, or psychological, play a large role in undermining mental health. Unhealthy lifestyle choices contribute significantly to high rates of obesity, cardiovascular diseases, eating disorders, anxiety, and mental disorders.
SOCIAL & COMMUNITY NETWORKS
Social and community networks is the next level in this model. This area focuses on the importance of a support system whether it’s family, friends or neighbors. This network of individuals make up the social circle with people within once community. Generally, people who are isolated and do not have much community interaction are more likely to develop mental health issues. Getting involved in the community through volunteer work, religious activities, and attending social gatherings can help one feel more connected, content, and happier. There is a stigma attached to mental illness that creates serious barriers in identifying, accepting, and getting treated for mental illnesses. This model acknowledges the importance of a support system outside of health care to evoke the best health outcomes.
LIVING & WORKING CONDITIONS
The next level comprises a large spectrum of factors including day to day activities, working conditions, education, housing, water, and sanitization, etc. The intertwining relationships between these factors make the situations more complicated. Homelessness, lack of affordable housing, and unemployment, further reduces the chances of access to healthcare resources. Homelessness coupled with addictions leads to high rates of mental health issues, and suicidal tendencies. These people further experience several barriers to getting education, finding employment, and accessing proper housing that further builds on to the burden of mental health.
(Centre for Addiction and Mental Health, 2020)
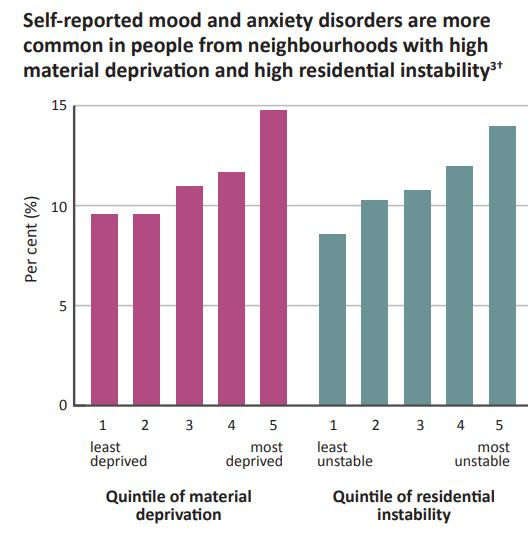
The image on the left graphically depicts the % age of mood and anxiety disorders recorded in 2011- 2012 amongst Ontarians.
A drastic rise in graph is recorded in population belonging to the high material deprived and high residential instable populations.
Thus we can conclude that communities belonging to the lower social and economic positions are more likely to be exposed to the negative impacts of the social and environmental factors.
CULTURAL AND ENVIRONMENTAL FACTORS
Finally, the last level of this model comprises of the general socio-economic, cultural and environment conditions. They can be understood as any factors that would impact health decisions and availability, access to transportation services, and clean air.
Mental illnesses are more prevalent in the Indigenous Canadians. There are multiple factors that have led to the challenges with mental health, higher rates of suicide, and substance abuse in this population. Some of the contributing factors are: centuries of victimization, poverty, poor rural infrastructure, gaps in services, and the lack of delivering culturally safe treatment options. There is a desperate need to create mental health programs and services in coordination with the elders of the Indigenous communities that align with their cultural believes and knowledge.
Centre for Addiction and Mental Health. (2020)
In this CBC article 'We are dying': Maskwacis community members overwhelmed by suicides" the author tries to look for answers after the community witnessed 14 deaths by suicide in less than 2 months. Click on the image for the full article.
(Morin, 2018)
(Knaak et al., 2017)
Mental illness-related stigma at all levels in all communities should be acknowledged. Although the intensity might be more for certain communities. This stigma especially in the healthcare sector creates a barrier to providing quality health care to our patients. Lack of awareness, stereotyping, unconscious bias further aggravates the problem.
Qualitative research has found that for many healthcare providers, it is only through the experience of receiving anti-stigma training that they become aware of the subtle and unintended ways certain beliefs and behaviours may have been contributing to stigmatizing experiences among their patients.
(Knaak et al., 2017)
As health care leaders it is very important to remove barriers through stigma reduction programs, workshops and training. Outreach to all communities and getting them involved in the decision- making process and planning intervention therapies would have a great impact.
CONCLUSION
It is true to state that mental illness affects people of all ages, genders, cultures, educational levels, and socio-economic backgrounds. Thus, we can safely conclude that one strategy will not fit all models of healthcare. There are certain factors that when combined increases the likelihood of impacting mental health negatively. The wider determinants of health model can be used to identify the gaps in services and barriers to achieving good mental health.
Mental illnesses can be treated effectively, so it is very crucial for the policy makers, health boards, and researchers to work together and build collaboration and partnerships between community partners in order to address factors on each level of the framework.
Programs and services should be tailored according to the needs and demands of each sector in the society. More partnerships & collaborations between government agencies, general public, and community groups can increase awareness and reduce discrimination and health inequalities in society regarding mental illnesses.
The Canadian Mental Health Associations Ontario has partnered with several provincial and local community partners to develop programs and healthcare services to help Ontarians combat with mental illnesses. The image below is linked to the list of resources available.
REFERENCES
Barras, M. (2018). A Statistical Report on the State of Indigenous Mental Health in Canada. Amnesty.
Canadian Council on Social Determinants of Health. (2015). A Review of Frameworks on the Determinants of Health. Canadian Council on Social Determinants of Health.
Canadian Mental Health Association. (2020). Mental Health.
Canadian Mental Health Association. (2020). Mental health: What is it, really?
Canadian Mental Health Association. (2020). Provincial Mental Health Supports
Centre for Addiction and Mental Health. (2020). Mental Illness and Addiction: Facts and Statistics
Knaak, S., Mantler, E., & Szeto, A. (2017). Mental illness-related stigma in healthcare: Barriers to access and care and evidence-based solutions. Healthcare management forum, 30(2), 111–116. https://doi.org/10.1177/0840470416679413
Morin, B. (2018). 'We Are Dying': Maskwacis Community Members Overwhelmed by Suicides. CBC News.
Public Health Ontario. (2014). Ontario Health Profile: No Health without Mental Health.
Public Health Ontario. (2019). Homelessness and Health Outcomes: What are the associations?






Comments